Previous Issues Volume 3, Issue 1 - 2018
Improvements in Gait Following Controlled Body Weight Suspension for a Person with a Transfemoral Amputation.
Judith A. Woehrle
Physical Therapy Program, Midwestern University, 19555 N 59th Ave. Glendale, Arizona 85308, United States of America.
Corresponding Author: Judith A. Woehrle, Physical Therapy Program, Midwestern University, 19555 N 59th Ave. Glendale, Arizona 85308, United States of America, Tel: 623-572-3921; E-Mail: [email protected]
Received Date: 06 Jan 2018 Accepted Date: 31 Jan 2018 Published Date: 02 Feb 2018
Copyright© 2018 Judith A. Woehrle
Citation: Woehrle JA. (2018). Improvements in Gait Following Controlled Body Weight Suspension for a Person with a Transfemoral Amputation. Mathews J Orthop. 3(1): 018.
ABSTRACT
Background and Purpose: Gait deviations are a common problem observed in a patient while using a lower extremity prosthesis. The purpose of this case report is to describe rehabilitation techniques including proprioceptive facilitation techniques with body weight suspension to improve gait speed, cadence, step length, and stance time for an able-bodied person who had a transfemoral amputation. Case Report: This case report describes pertinent information addressing interventions for a patient with a left transfemoral amputation due to cancer. Outcome measures were taken prior to and following six sessions of interventions. The patient’s primary goal was to improve gait, which will help with walking greater distances with ease among a crowd of people.
Conclusion: Improvements were found with gait speed, step length, ambulation time, and step length differential. The most important factors in rehabilitation to improve gait parameters such as speed, cadence, and step length, are to ensure that the person has the ability to lift the prosthesis using the residual limb, control step length and foot placement with the prosthetic limb using timing and proprioceptive feedback while walking. The patient in this case had successful improvements following a protocol that emphasized lifting and timing of the prosthetic limb while walking.
Keywords: Above Knee Amputation; Body Weight Suspension; Rehabilitation; Gait; Gait Speed; Cadence; Body Weight Suspension.
INTRODUCTION
There are 1.8 million Americans who are living with amputations of the leg, which includes 1,631 US Service Members who sustained amputations from 2001 through July 2011[1]. Amputations result from trauma, diabetes, peripheral vascular disease, frostbite, infections, and tumors. Community ambulation is a typical functional goal, for individuals with lower limb amputations, that includes navigation of various terrains and surface angles. People with lower limb amputations have a fear of falling or have had a history of falls [2]. Risk factors that attribute to falls are comorbidities, medications, vascular disease, age, vision, mental status, and muscle weaknesses [2,3]. People with a transfemoral amputation (TFA) are at a greater risk of falling than those with an amputation below the knee [2]. While walking with a prosthesis, the majority of people will exhibit gait deviations to compensate for muscle weakness, unsteadiness, and fear of falling. It is important that a specific rehabilitation program is designed to address gait deviations while walking with a prosthesis, which in turn might help the person become more confident and prevent falls
There are no known protocols; however, there are variations of some treatments to address gait deviations for people who use a prosthesis. Addressing stability, weaknesses, and mobility by way of exercises and perturbation-based gait training have improved walking abilities of people using a prosthesis [4]. Another rehabilitation technique, to change gait, is the use of a treadmill with body weight suspension. In normal able-bodied people it was found that by unloading the body, changes will occur with cadence, step length, and stride lengths, thus effecting speed [5, 6, 7]. Hip flexors are needed to accelerate the leg into a forward momentum during double limb support. Depending upon the type of prosthetic knee, a person with a TFA requires strong hip extensors to keep the knee extended in stance due to the loss of needed sensory motor function to control the position of the prosthetic knee and ankle [8]. In an able-bodied person without a TFA, knee flexors and extensors are coactivating to stabilize the knee during initial contact (IC). The calf muscles contract restraining the tibia from advancing to stabilize the knee during loading response (LR) and remain contracting to control the tibia through terminal stance (TS). This mechanism of control allows the femur to advance faster than the tibia beginning at midstance (MS) [9, 10]. Without these mechanisms of control, a person with a TFA will depend upon and require specific timing and strength of the surrounding hip muscles.
This case report describes the effect of rehabilitation using proprioceptive facilitation techniques such as touch and tapping for hip flexion and abduction during weight bearing and forward momentum of the leg while off of a treadmill and with body weight suspension while on a treadmill for an ablebodied person with a TFA. The aim of this case report is to determine whether the rehabilitation techniques administered during treatment sessions will improve gait speed, cadence, step length, and stance time on the prosthetic side.
CASE REPORT
The patient is a 62 y/o Caucasian female (height = 1.68m, weight = 87.3kg) who had a left mid TFA in 2012 due to cancer. Comorbidities include a history of chondrosarcoma of the knee with multiple surgeries. She is not taking any prescribed medications. She has participated in physical therapy off and on since her amputation. She has been an independent prosthetic ambulator for the past 5 and a half years, is active in the community, plays Bocce Ball with a team once a week, and travels locally and abroad. She will use a cane while ambulating in the community for support, security, and fear of falling or losing her balance among a crowd of people. In her home, she ambulates without a cane.
The patient has received a couple of different components for her leg since her amputation. The components that she had during her visits were a socket with a one-way expulsion valve to allow passive suction, silicone liner, cotton liner over the residual limb (for perspiration),Rheo® knee and a Kinterra foot. She complained of difficulty walking for long distances, such as in the mall, and when her ankle and foot become sore on the sound side, she would know that it is time to rest. When she became tired, she noticed that her left prosthetic foot would scrape the floor. Her goals are to feel more confident walking without her cane, improve her gait which could be contributing to her back pain especially after walking long distances, clear her toes on the prosthetic side, increase stance time on the prosthetic leg while walking, and walk longer and easier among a crowd of people.
EXAMINATION
Prior to intervention, the functional measurements taken were the Timed-Up-and-Go (TUG), Single Leg Stance Test (SLS), functional muscle strength testing, and gait analysis for 6 footfalls using the GaitRite® system to establish a baseline. Two testers administered the tests showing reliability within and between testing using intraclass correlational coefficients (ICC) values ranging from 0.99-0.98. The TUG is a simple and practical tool that is reliable and useful to determine a person’s functional mobility and risk for falls [11-15]. It is predicted that an individual who took up to 13 or 14 seconds to complete the TUG test, that person had respectively, a 69% and an 83% probability of being a faller [13]. The mean after 3 trials of TUG was 15.33 (SD=0.47) seconds. The patient used a straight cane and demonstrated stability while walking around the cone and turning to sit in a chair with arm rests.
SLS trials are recorded in Table 1 with the mean of 1.12 (SD = 0.130) seconds on the left prosthetic leg and 14.84 (SD = 5.970) seconds on the sound leg. Using SLS provides a reliable method to detect balance impairments. It was found that as a person ages, it becomes more difficult to stand on one limb with both eyes opened or closed [16].
Table 1: Single Leg Stance Test (SLS) – measured in seconds.
| (Prosthetic limb) SLS– tester 1 | (Prosthetic limb) SLS– tester 2 | (Sound side) SLS– tester 1 | (Sound side) SLS – tester 2 |
|---|---|---|---|
| 1.16 | 1.07 | 9.27 | 9.3 |
| 0.93 | 0.88 | 13.87 | 13.84 |
| 1.28 | 1.15 | 23.94 | 23.88 |
| 1.25 | 1.16 | 18.31 | 18.13 |
| 1.18 | 1.19 | 8.96 | 8.91 |
Functional muscle strength testing was determined by asking the patient to lift her prosthetic leg in a sagittal plane while standing and while in a seated position with the hip bent to a 90° and to an approximate 30°position to determine the strength of hip flexors. She exhibited functional weakness of the hip flexors in all positions. To initiate momentum for this motion in all positions, she would lean her trunk backward in an attempt to raise the prosthetic limb. While standing, she exhibited a pelvic drop on the right side. This posture provides an example of either gluteus medius weakness or global weak- ness of the muscles that abduct the hip [17]. The patient's ability to move the prosthetic limb backwards, in a sagittal motion, was performed without using momentum from her trunk muscles; therefore, she had the capability of using the gluteus maximus muscle with minimal effort while standing. Hip flexor tightness was noted on her left hip while standing. She was able to actively maintain neutral position of the left hip, with assistance from examiner to keep pelvis in neutral.
The GAITRite® system is a reliable and valid tool that measures temporal and spatial parameters of gait [18-20]. The GAITRite® system is a computerized instrumented walkway, which is padded, is five meters in length, and has sensor pads embedded within the walkway. The sensors capture each footfall as a function of time. The system continuously scans the sensors while the person walks on the walkway. Data is transferred to a personal computer that processes and calculates information into footfall patterns and gait characteristics. The patient walked on the walkway 4 times without her cane. Parameters of gait were averaged and recorded in Table 2. This system was used as an outcome measure to determine whether gait speed, cadence, and step length improved after interventions.
Prior to intervention, the functional measurements taken were the Timed-Up-and-Go (TUG), Single Leg Stance Test (SLS), functional muscle strength testing, and gait analysis for 6 footfalls using the GAITRite® system to establish a baseline. Two testers administered the tests showing reliability within and between testing using intraclass correlational coefficients (ICC) values ranging from 0.99-0.98. The TUG is a simple and practical tool that is reliable and useful to determine a person's functional mobility and risk for falls [11-15]. It is predicted that an individual who took up to 13 or 14 seconds to complete the TUG test, that person had respectively, a 69% and an 83% probability of being a faller [13]. The mean after 3 trials of TUG was 15.33 (SD=0.47) seconds. The patient used a straight cane and demonstrated stability while walking around the cone and turning to sit in a chair with arm rests.
SLS trials are recorded in Table 1 with the mean of 1.12 (SD = 0.130) seconds on the left prosthetic leg and 14.84 (SD = 5.970) seconds on the sound leg. Using SLS provides a reliable method to detect balance impairments. It was found that as a person ages, it becomes more difficult to stand on one limb with both eyes opened or closed [16].
Table 2: GAITRite® parameters – initial examination (Day 1).
| Parameters | Prosthetic side (left) | Sound side (right) | Parameters | Data |
|---|---|---|---|---|
| Step Length | 54.22cm | 60.83cm | Ambulation Time | 3.84 sec |
| Stride Length | 115.18cm | 112.67cm | Velocity | 89.9 cm/ sec |
| Single Support | 27.3cm | 45.0cm | Cadence (steps/ min) | 93.8 steps/ min |
| Swing Time (% of gait cycle) | 44.70% | 27.50% | Step Length Differential | 6.62 cm |
| Stance Time (% of gait cycle) | 55.30% | 72.50% |
As the patient was observed while walking, during the phase of MS, which requires the center of mass to pass over a stable base, she would take less stance time on the left prosthetic leg since she was concerned about balance and unsteadiness. During MS on the left prosthetic leg, the pelvis on the right side would drop and the trunk would bend left. The patient would inconsistently drag the left prosthetic foot across the surface during initial swing (IS), which was observed most often when the patient said that she was either tired or unable to concentrate.
Clinical Impressions and Prognosis Several functional deficits were found during the initial examination. TUG scores were low, indicating that the patient remained at risk for falls. With SLS, the patient was able to stand longer on the sound leg than on the prosthetic leg, showing deficits with balancing on the prosthetic leg. The inability to maintain a longer time standing on the prosthetic leg influences stance time while walking. The patient was more dependent on the sound leg when walking which causes her to stop walking and rest. Gait parameters such as step length and single support are unequal and step length differential is just over 6cm as noted in Table 2. Functional strength is diminished for the hip flexors and abductors on the prosthetic side
The patient has had a prosthesis for five and a half years and has received rehabilitation off and on for the past five years. She has had more than one prosthesis since her amputation and is considered a Medicare K3 functional level. The prognosis for this case is good since this patient has had previous rehabilitation and was cognizant of her gait pattern and the necessary changes needed to improve cadence and gait speed.
INTERVENTIONS
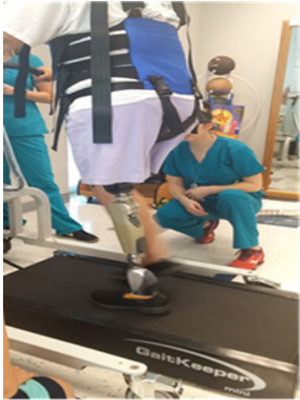
After being introduced to the body weight suspension system (Figure 1), the patient was taught to place emphasis on shifting weight on to the prosthetic leg keeping the trunk upright over the pelvis with 50% to 81% weight bearing on the prosthetic limb with the idea of changing the temporospatial and kinematic patterns of the hip, on the prosthetic side, while walking. Treadmill speed was kept at 0.58-0.60m/s which was considered comfortable for the patient. Keeping the treadmill speed at 0.58-0.60m/s did not cause the patient to fatigue. Setting the treadmill at 0.58-0.60m/s was comparable to the speeds used in various studies designed for people with amputations while using 50-20% of body weight suspension [6, 7, 21, 22]. Proprioceptive facilitation techniques using touch and tapping was provided to the surrounding hip muscles on the prosthetic side, while on the treadmill, to assist the patient with advancement of the prosthetic leg for a greater step length and consistent heel strike (Table 4/Days 3, 4, 5, 6). Static standing activities and forward movement of the prosthetic limb by stepping over an object while keeping the pelvis and trunk level was repeated in the parallel bars (Table 4/Days 4, 5). Isometric contractions of the hip muscles were emphasized while standing and at the same time the trunk had to be in the upright position over the pelvis. Detailed interventions are outlined in Table 3 addressing techniques emphasized and used on and off of the treadmill.
Table 3: Interventions – 6 visits for rehabilitation.
| Day | Gait with cane on level surfaces; intro to BWS | BWS (off of treadmill) with weight shifting to prosthetic side | Right hip hiking on BWS (off of treadmill) | BWS on treadmill at 0.58-0.60 m/sec using verbal cueing for (L) hip flexion | Proprioceptive facilitation(tapping and touch)(L) knee and hip flexion; assisting with toe off, step length, heel strike, and pelvic alignment on (L) prosthetic side | Isometric(L) glute medius exercise with towel roll under (L) residual limb | (L) hip flexion stretch with patientsupine on mat | Prone lying, passive (L) hip extension of residual limb with pelvic stabilization | Standing in parallel bars, foam square with height of 2 1/2� in front of patient |
|---|---|---|---|---|---|---|---|---|---|
| 1 | X | ||||||||
| 2 | X | X 79% WB on(L) prosthetic leg | X | ||||||
| 3 | X 79% WB with 1” lift under (L) prosthetic foot | X added toe off and preswing with (L) prosthetic foot at 73% WB | X | X 3 x 10 reps | X using contract/relax technique | X | |||
| 4 | X 60% WB with 1” lift under (L) prosth | X added initial contact with (L) prosthetic foot at 50-60% WB | X 3 x 10 reps | X step up with (L) prosthetic foot on foam square x10 with 50% of trials completed successfully | |||||
| 5 | X 60-100% WB with straight cane with breathing techniques | X weight shifting with 100% WB, holding on to the BWS handle bars | X added step length, heel contact, knee flexion, and toe off on (L) prosthetic leg with 70% WB | X | X 3 x 10 reps | X repeated same as day 4 with 80% trials completed successfully | |||
| 6 | X 100% WB then 80% WB while holding on to the BWS handle bars | X added knee flexion during terminal stance and preswing on (L) prosthetic leg with 80-90% WB | X |
Abbreviations: BWS, body weight suspension; WB, weight bearing; (L), lef
Figure1: Body weight suspension systemset-up.
RESULTS
During the six visits of intense intervention, the patient did show some improvements in gait parameters, as measured with the GaitRite® (Table 4). Since the initial examination, improvements were with step length, cadence, velocity, and step length differential over time. Step lengths were nearly equal (left = 58.82cm, right = 58.26cm), cadence improved 4%, velocity increased 6%, and step length differential over time changed 92% since the initial examination, which is indicative of overall improved step length. There were positive changes in swing time and stance time on the prosthetic side after six visits. The patient was able to voluntarily move each lower extremity at an even and faster pace. Stride lengths changed since the initial exam.
Table 4: GaitRite® Parameters - final visit (Day 6).
| Parameters | Prosthetic side (left) | Sound side (right) | Parameters | Data |
|---|---|---|---|---|
| Step Length | 58.22cm | 58.26cm | Ambulation Time | 3.68 sec |
| Stride Length | 27.5cm | 43.5cm | Velocity | 95.4 cm/ sec |
| Single Support | 27.7cm | 27.5cm | Cadence (steps/ min) | 97.8 steps/ min |
| Swing Time (% of gait cycle) | 57.10% | 72.10% | Step Length Differential | 0.56 cm |
| Stance Time (% of gait cycle) | 58.82% | 58.26% |
Functional deficits remained after testing strength of the hip flexors (iliopsoas) and hip abductors (gluteus medius) on the prosthetic side. The patient demonstrated difficulty raising her left prosthetic foot off of the floor while seated and standing due to weakness and fatigue. While she stood on her left leg, holding on to a surface for balance, hip drop was seen on the right side. TUG measurements improved to a mean of 13.88 (SD=0.37) seconds but the patient remains at risk for falls [13]. SLS measurements on the left remain low, compared to the right side, and did not improve since the initiation of the interventions.
DISCUSSION
This case report describes the effect of rehabilitation, using techniques to facilitate hip strengthening on and off of a treadmill using body weight suspension and proprioceptive facilitation techniques for the hip and trunk for an able-bodied person with a TFA. The techniques that were chosen for this particular case were based upon patient goals, observation of gait with a prosthetic limb, and results from the initial outcome measures. This patient's goals were to feel more confident walking without her cane, improve her gait which could be contributing to her back pain especially after walking long distances, clear her toes on the prosthetic side, increase stance time on the prosthetic leg while walking, and walk longer and easier among a crowd of people.
Emphasis was placed upon the hip, prosthetic knee and foot throughout the gait cycle. During phases of gait, proprioceptive facilitation techniques were used in the form of touch and tapping focusing on the hip muscles for the purpose of facilitating muscle contraction. During IS the patient needed to rely on the hip flexors to initiate the necessary momentum to swing the leg forward [9,10]. Since the patient had a midfemoral amputation, she no longer had muscles such as the rectus femoris, adductor longus, gracilis, and sartorius peak in activity during IS. The concentric contraction of these muscles along with the iliacus and iliopsoas are needed for generating momentum for hip flexion to maintain the femur in midline [10]. During double limb support, hip flexors are needed to accelerate the leg into a flexion moment [8]. Without strong hip flexors, people with a TFA have a fear of loading onto the prosthetic limb causing greater muscle force in the trunk muscles to assist with toe clearance of the prosthetic limb [23]. One of the patient's goal was to correct the tendency to drag her toes on the prosthetic side. To address her goal, it was necessary to concentrate on strengthening the hip flexors on the prosthetic side, lifting the leg high enough to clear the foot. The inability to clear the prosthetic foot consistently, while walking, becomes difficult especially if the person becomes fatigued. The patient attempted to place greater stance time on the sound side to shift her center of mass, initiating momentum from the trunk and hip flexors to swing the prosthetic limb forward. Due to weakness of the hip flexors and abductors on the prosthetic side the patient demonstrated less single support time and overall less stance time on the prosthetic limb, which could influence balance.
The intervention concentrated on facilitating the hip flexors and abductors while using the controlled body weight suspension system. With body weight suspension, the patient was able to concentrate on the motion of the prosthetic leg and carry the weight of the prosthetic limb during forward progression using the iliopsoas muscle. People with a TFA have a muscle mass of 30% of a normal lower extremity but need to generate enough hip flexor momentum similar to a normal leg for forward progression of the limb during gait. Stance time also decreases with body weight suspension [7]. Adjusting treadmill speed using body weight suspension will change cadence, stride length, and stance time if less than 50% of body weight unloading is used during treatment [5]. Another change that occurs with use of body weight suspension on the treadmill is hip flexion range of motion (ROM) [6]. The greater the amount of body weight unloading used during IC, the less hip flexion ROM is needed during treadmill walking. During toe off there is no difference in hip angle between 10%, 50%, and 70% body weight suspension; however, during IC, as the amount of body weight suspension increased, the hip maximum angle decreased. Stride lengths changed since the initial exam. It was found that the patient had shorter stride lengths following 6 interventions but cadence improved (steps/minute). The patient was able to voluntarily move each lower extremity at an even and faster pace. It is speculated that the diminished stride lengths are due to the idea that the patient took more steps per minute to increase velocity. Shorter steps might have given the patient a feeling of security while advancing the sound side and placing weight on the prosthetic side during single limb stance.
CONCLUSION
The treatment designed for this particular patient could be replicated using a body weight suspension system. For example, in a randomized controlled trial, investigating the efficacy of using a body weight suspension system for able-bodied people with a TFA to improve gait parameters over time would be useful especially for rehabilitation purposes. Testing patients with a TFA to determine whether the residual limb is strong enough to lift the prosthetic components against gravity and reinforcing new methods of walking while encouraging appropriate use of muscles is important during rehabilitation. Functional strength is necessary for anyone who has had a TFA especially if there is a need to walk long distances without fatigue while using a prosthesis. Determining the functional strength of the residual limb and carefully examining gait should be considered upon the initial examination.
REFERENCES
- Krueger CA, Wenke JC and Ficke JR. (2012). Ten years at war. J Trauma Acute Care Surg.73(6): S438-S444.
- Miller WC, Speechley M and Deathe B. (2001). The prevalence and risk factors of falling and fear of falling among lower extremity amputees. Arch Phys Med Rehabil. 82(8): 1031-1037.
- Hunter SW, Batchelor F, Hill KD, Hill A-M, et al. (2017). Risk factors for falls in people with a lower limb amputation: a systematic review. PM&R. 9(2): 170-180.
- Sheehan RC, Rabago CA, Rylander JH, Dingwell JB, et al. (2016). Use of perturbation-based gait training in a virtual environment to address mediolateral instability in an individual with unilateral transfemoral amputation. Phys Ther.96(12): 1896-1904.
- Ruckstuhl H, Kho J, Weed M, Wilkinson MW, et al. (2009). Comparing two devices of suspended treadmill walking by varying body unloading and Froude number. Gait Posture. 30(4): 446-451.
- Threlkeld AJ, Cooper LD, Monger BP, Craven AN, et al. (2003). Temporospatial and kinematic gait alterations during treadmill walking with body weight suspension. Gait Posture.17(3): 235-245.
- Awai L, Franz M, Easthope CS, Vallery H, et al. (2017). Preserved gait kinematics during contolled body unloading. Journal of NeuroEngineering and Rehabiliation.14(25): 1-10.
- Czerniecki JM. (1996). Rehabilitation in limb deficiency. 1. Gait and motion analysis. Arch Phys Med Rehabil. 77(3): S3-S8.
- Perry J and Burnfield JM. (2010). Gait Analysis: Normal and Pathological Function. In: Perry J, Burnfield JM. Hip. 2nd ed. Thorofare, NJ: SLACK Inc. 103-120.
- (2001). The Pathokinesiology Service & Physical Therapy Department, Rancho Los Amigos National Rehabilitation Center. Observational Gait Analysis Handbook. Downey, CA: Los Amigos Research and Education Institute. Rancho Los Amigos National Rehabilitation Center
- Fuenzalida Squella SA, Kannenberg A and Brandao Benetti Â. (2017). Enhancement of a prosthetic knee with a microprocessor-controlled gait phase switch reduces falls and improves balance confidence and gait speed in community ambulators with unilateral transfemoral amputation. Prosthet Orthot Int.;1(00(0)): 1-8.
- Mathias S, Nayak US and Isaacs MD. (1986). Balance in elderly patients: The “get-up and go” test. Arch Phys Med Rehabil.67(6): 387-389.
- Shumway-Cook A, Brauer S and Woollacott M. (2000). Predicting the probability for falls in community-dwell-ing older adults using the Timed Up & Go Test. Phys Ther.80(9): 896-903
- Podsiadlo D and Richardson S. (1991). The timed “Up & Go”: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc. 39(2): 142-148.
- Clemens SM, Gailey RS, Bennett CL, Pasquina PF, et al. (2017). The Component Timed-Up-and-Go test: the utility and psychometric properties of using a mobile application to determine prosthetic mobility in people with lower limb amputtions. Clin Rehabil.
- Springer BA, Marin R, Cyhan T, Roberts H, et al. (2007). Normative values for the unipedal stance test with eyes open and closed. J Geriatr Phys Ther.30(1): 8-15.
- Fujita K, Kabata T, Kajino Y, Iwai S, et al. (2017). Quantitative analysis of the Trendelenburg test and invention of a modified method. J Orthop Sci. 22(1): 81-88.
- Menz HB, Latt MD, Tiedemann A, Kwan MMS, et al. (2004). Reliability of the GAITRite® walkway system for the quantification of temporo-spatial parameters of gait in young and older people. Gait Posture.20(1): 20-25.
- Webster KE, Wittwer JE and Feller JA. (2005). Validity of the GAITRite® walkway system for the measurement of averaged and individual step parameters of gait. Gait Posture. 22(4): 317-321.
- Bilney B, Morris M and Webster K. (2003). Concurrent related validity of the GAITRite® walkway system for quantification of the spatial and temporal parameters of gait. Gait Posture. 17(1): 68-74
- Darter BJ and Wilken JM. (2011). Gait training with virtual reality-based real-time feedback: improving gait performance following transfemoral amputation. Phys Ther. 91(9): 1385-1394.
- . Mikami Y, Fukuhara K, Kawae T, Kimura H, et al. (2015). The effect of anti-gravity treadmill training for prosthetic rehabilitation of two cases with lower limb amputation. Prosthet Orthot Int.39(6): 502-506
- Shojaei I, Hendershot BD, Wolf EJ, et al. (2016). Persons with unilateral transfemoral amputation experience larger spinal loads during level-ground walking compared to able-bodied individuals. Clin Biomech.32: 157-163.