Previous Issues Volume 1, Issue 2 - 2016
Case Report the Muscle Loss in the Intra Operative Strabismus Surgery
Luma Pinheiro E Pinho1,Jorge Antônio Meireles Teixeira1,Gian Francisco Rodrigues Cooper Dos Santos1,Reinaldo Izidório dos Santos Filho1,Álvaro Bruno Botentuit Serra de Castro1,Samira Gracielle Pinheiro Cutrim1,Julia Brandão de Paiva Teixeira Custódio1,José Daniel Aguiar Costa1
1Hospital Universitário Presidente Dutra, São Luís-Maranhão, Brasil.
Corresponding Author: Luma Pinheiro e Pinho, Hospital Universitário Presidente Dutra, São Luís-Maranhão, Brasil, Tel: 98-984136173; E-Mail: [email protected]
Received Date: 11 Feb 2016 Accepted Date: 26 Dec 2016 Published Date: 29 Dec 2016
Copyright © 2016 Pinho LPE
Citation: Pinho LPE, Teixeira JAM, Santos GFRCD, Filho RIDS, et al. (2016). Case Report the Muscle Loss in the Intra Operative Strabismus Surgery. Mathews J Ophthalmol. 1(2): 010.
INTRODUCTION
A lost muscle is one of the most devastating complications that a strabismus surgeon can face in the intra-operative period. Rectus muscles can be lost due to trauma or surgery, including sinus surgery, strabismus surgery, and other ocular surgeries [1-3]. A lost medial rectus muscle is usually expected in the presence of an overcorrection after exotropia surgery or under correction after exotropia (XT) surgery, resulting in limited duction in the field of action of the muscle. If not treated, a lost muscle will lead to consecutive strabismus, diplopia, and a large limitation of eye movement in the direction of the lost muscle [4].
OBJECTIVE
To report the intraoperative loss of the medial rectus muscle during strabismus surgery and posterior treatment.
CASE REPORT
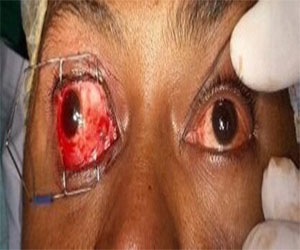
A 31 years old man, native of Sao Luis, was referred to the strabismus service due to XT complaints ever since the age of 10, in addition low vision in the right eye. On ophthalmological examination was verified best-corrected visual acuity 0.05/1.0; with preference for the left eye. Concerning extrinsic eye muscles presented XT 25^ concomitant. On monocular rotation tests we found +2 right lateral rectus with ametropic in both eyes. Bio microscopy and funduscopy unaltered in both eyes. The surgical plan was 6.0 mm right medial rectus (MR) resection and a 5.0 mm withdrawal of the right lateral rectus. Due to its friability and lack of support for suturing, the right MR muscle was lost during surgery. Therefore, a transposition of superior rectus to the MR was performed, using a technique similar to that of Jensen’s. The post-operative results after a month were XT 40 (on Hirschberg test) and -2 right medial rectus on monocular rotation tests, besides of normal bio microscopy and funduscopic evaluations (Figure 1).
Figure 1: Primary Position of Gaze. Exotropia in Right Eye After First Intervention.
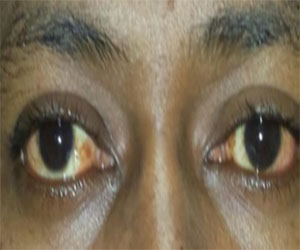
Upon six months of post-operative, the patient presented concomitant XT 25^ and 12 of right hypertropia (on Krimsky test) and -2 right MR on monocular rotation. One year after the first surgery, a second approach was done with the initial plan being. It was receded right lateral rectus 12.0mm plus 1.0mm anterior dislocation of the right lower oblique ahead of the right inferior rectus (peribulbar). However, due to the increased risk of anterior chamber ischemia, a triple marginal myotomy was performed on the right lateral rectus including anterior dislocation right lower oblique (1.0mm ahead of the right inferior rectus edge) and innervation (recede of the left lateral rectus 8.0 mm). On the seventh post-operative day, the patient presented XT 12^ with right hypertropia 10^, monocular rotation tests showed -2 and -3 right MR and -2 right lateral rectus. Three months after the second intervention, the patient displayed good healing, right hypertropia 15ˆ, and -2 right lateral rectus and -2 right MR (Figure 2), monocular rotation tests with the patient now being discharged.
Figure 2: Primary Position of Gaze. Right Eye: After Second Intervention Showing Reduction of XT Deviation.
DISCUSSION AND CONCLUSION
A lost muscle means no attachment to the globe. Plager and Parks reported that 67% of lost superior, inferior, and lateral rectus muscles were retrievable while only 10% of lost MR muscles were retrievable [3]. MacEwen et al. found that MR muscles that were cut and lost during strabismus surgery are seldom located, but snapped or traumatically severed muscles are frequently located [4]. Several surgical options are available after surgical loss of a MR muscle. An isolated lateral rectus recession has a significant possibility of considerable under correction of the typical large-angle exotropia associated with this challenging complication of strabismus surgery. Combined vertical transposition to MR and lateral rectus recession increases the risk of anterior segment ischemia [5, 6]. Cho et al. treated 4 patients with exotropia and limited adduction following sinus surgery with an X-type of transposition in which each half-tendon is pulled and crossed through the under surface of the severed MR to the other end of the MR insertion. Two of 4 patients underwent concurrent lateral rectus recession depending on the result of the forced duction test. In the two cases in which lateral rectus recession was done, one was orthophoria and the other had a residual XT of 70 prisms and adduction deficit that the authors attributed to adhesions around the lateral rectus. Only 1 patient in this series of 4 appeared to benefit from lateral rectus recession [7]. In conclusion, cases such as this, in which there is muscle loss during the first strabismus intervention with concomitant intra- operative attempt of superior rectus to MR transposition without success, awaiting healing is preferable due to the friable nature of the muscle, with posterior treatment using the triple marginal myotomy procedure, anterior dislocation and innervation, which proved to be efficacious in the correction of the deviation, preserving later versions.
REFERENCES
- Hamlet YJ, Goldstein JH and Rosenbaum JD. (1982). Dehiscence of the lateral rectus muscle following intrascleral buckling procedure. Ann Ophthalmol. 14(7), 694-697.
- Murray AD. (1998). Slipped and lost muscles and other tales of the unexpected. Philip Knapp Lecture. J AAPOS. 2(3), 133-143.
- Plager DA and Parks MM. (1990). Recognition and repair of the ‘‘lost’’ rectus muscle. A report of 25 cases. Ophthalmology. 97(1), 136-137.
- MacEwen CJ, Lee JP and Fells P. (1992). Aetiology and management of the ‘detached’ rectus muscle. Br J Ophthalmol. 76(3), 131-136
- Cho YA and Won JS. (1995). Two cases of anterior segment isch-mia after strabismus surgery. J Korean Ophthalmol Soc. 36, 97-102.
- Elsas FJ and Witherspoon CD. (1987). Anterior segment ischemia after strabismus surgery in a child. Am J Ophthalmol. 103(6), 833-834.
- Cho YA, Rah SH, Kim MM and Lee JY. (2008). Vertical rectus muscles transposition in large exotropia with medial rectus muscle transection following endoscopic sinus surgery. Korean J Ophthalmol. 22(2), 104-110.