Previous Issues Volume 1, Issue 2 - 2016
Reading Glasses to Prevent Myopia
Peter R Greene1 ,Otis S Brown2 ,Vladimir Medved3,Zachary W Grill4
1B.G.K.T. Consulting Ltd. Bioengineering Huntington, New York.
2Optics, C & O Research Waynesboro, Penn.
3Faculty of Kinesiology, Electrical Engineering & Computing, University of Zagreb, Croatia.
4Psychology Temple University Philadelphia, Penn.
Corresponding Author: Peter R Greene, B.G.K.T. Consulting Ltd. Bioengineering Huntington, New York, 11743, Tel: +1 631 935 56 66; E-Mail: [email protected]
Received Date: 29 Oct 2016 Accepted Date: 02 Nov 2016 Published Date: 15 Nov 2016
Copyright © 2016 Greene PR
Citation: Greene PR, Brown OS, Medved V and Grill ZW. (2016). Reading Glasses to Prevent Myopia. Mathews J Ophthalmol. 1(2): 008.
ABSTRACT
Preliminary experimental design using reading glasses at the U.S. Naval Academy at Annapolis are discussed. The conclusion is that (+) add lenses, used as reading glasses during study, can prevent the development of myopia for college students in pilot training.
KEYWORDS
Progressive Myopia; Reading Glasses; Bifocals; Progressive Add Lenses (PALS); Refraction; Myopia Prevention; Diopters.
INTRODUCTION
Literature Review
Cheng et al. [1, 2] (2011, 2014) and Gwiazda et al. and Hyman et al. [3, 3a, 4] (2003, 2005,2014) present a comprehensive listing of modern studies to date in terms of using (+) Add reading glasses to prevent or slow the progression of myopia. Brown & Berger (1979), Brown & Young (1981), Schaeffel & Howland (1988), Medina & Fariza (1993), and Greene, Brown, Medina & Graupner (1996) use first order control theory to predict myopia development as a function of time [5-9]. Thorn, Gwiazda & Held (2005) present a mathematical model of myopia development using the Gompertz function [10]. Hung & Ciuffreda (2007) develop IRDT, incremental retinal defocus, to explain myopia during the growth phase [11]. Medina et al. [12-14] (2015, 2016) and Greene & Medina [15-18] (2015, 2016) use control theory to explain myopia development, solved with digital and analog computer techniques to evaluate first-order equations. Viikari (2011) and Goldschmidt (2003) present comprehensive reviews of juvenile myopia, and various techniques used to control this myopia progression [19, 20]. Theories are many and varied, in terms of the causes of myopia [19, 20]. Figure 1a and 1b below show the nearwork demand problem, typical of college students, and the proposed optical solution to the problem, namely, custom reading glasses [21]. In this report, various mathematical control theories are reviewed, derived from conventional electrical engineering concepts, as shown in Figure 1c below:
Figure 1a: Norman Rockwell’s “The Law Student”, from the Saturday Evening Post, is seen reading at an effective distance of -3.0 to -4.0 diopters.
Figure 1b: Reading glasses for a -5.00 D. college myope. (+) Add technology is used by both bifocals and progressive addition lenses, “PAL’s”. PAL’s are “no-line” bifocals. Basically, these (+) Add reading glasses are distance compensators, with a +3.00 D Add for reading.
The Average Value of Accommodation
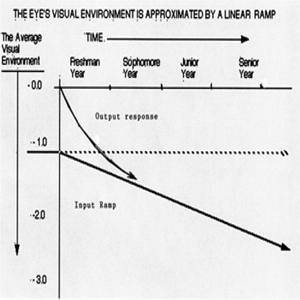
The controlling variable for this equation is the eye’s value of accommodation. The focal settings of the lens is determined by information decoded at the surface of the retina. The visual environment may be calculated by the use of the equation: VISUAL ENVIRONMENT = - 1 / (OBJECT DISTANCE) (In Diopters) (In Meters) A visual object moved inwards from infinity to one meter constitutes an environment change of - 1.0 diopters. Under this circumstance, the accommodation system will servo the lens by + 1.0 diopters to again achieve sharp focus at the surface of the retina. Visual Environment of College Students. As we enter higher academic institutions, our visual environment gradually shifts to a more negative value, as shown in Figure 1c below. We can characterize this increased “near” environment by the following ramp function:
Figure 1c: Ramp function A = m t + b
A = m t + b, where: A = Accommodation, daily average value, from the start of the freshman year. m = - 0.001 diopters / day = - 0.365 D/yr t = time in days b = - 1.0 diopters The Laplace transform of a unit ramp is: 1 / (s ^2) Applying this ramp to the eye’s transfer function produces: System’s Response = [m / s ^2] * [1 / (TAU s + 1)] The eye’s time domain response to a ramp function is 30: Focus = Offset Accommodation (Initial Value) (Ramp) + Accommodation * TAU [(t / TAU) - 1 + EXP (- t / TAU)]
DISCUSSION
Focal Status Produced by a Plus Lens
After two hundred days, this equation predicts that the eye will show the same linear slope as the accommodation ramp. We can logically expect that the eyes of college students will show a gradual movement towards, and eventually, into myopia when a linear ramp is applied to their accommodation system. How close does this scenario match the actual situation? In a study of the cadets at West Point, Dr. Gmelin determined that freshmen with 20/20 vision and 0 diopters focal state would, after four years, develop 20/80 vision with -1.3 diopters of myopia [22]. A similar study was conducted at the United States Naval Academy by Dr. Hayden, reviewed by Greene et al. [15, 16, 23, 24] (2015, 2016). This study showed an approximately linear change in focal status towards myopia in the eyes of almost all the normal eyed midshipmen [22, 25, 26]. Figure 1a shows Norman Rockwell’s classic painting “The Law Student”, from the Saturday Evening Post, where the student is seen reading at an effective distance of -3.0 to -4.0 diopters.
Myopia Prevention
We have plotted the historical development of myopia as a function of time, as shown in Figure 4d. The dynamic theory explicitly states that the eyes of the USNA midshipmen move into nearsightedness due to their increasingly confined visual environment. Their focal status change is in the right direction and proper magnitude to suggest quantitative verification for this dynamic model of the normal eye’s long-term behavior. If their myopia is a result of normal servoing action, a major means of changing this situation would be to use a convex lens for all close work. Use of this lens would substantially alter their visual environment from an estimated value of - 1.5 diopters, to a more reasonable figure of - 0.4 diopters. Their resulting focal status was calculated by the use of the equation developed [5, 6, 26].
CONCLUSIONS
Work done during the past twenty years has demonstrated that the accommodation system is a superb example of a physiological control system. It is a complex, sophisticated, and accurate system. We can logically expect that the normal eye will show equal competence in the design of its long-term control system. The process of building a mathematical model of a physiological system necessarily implies the idealization of that system. Models are not tested in a vacuum. The development of a servo-heredity model suggests an alternative model which we will call, for the purpose of identification and discussion, a “negative-lens-heredity” theory of the eye’s long-term focus. Heredity is a fundamental factor in both of these theories. There is a disagreement on how this factor establishes the eye’s long-term focus. These theories yield contradictory predictions that can be tested. The negative-lens theory predicts that:
- The eye’s focal status will not change due to a plus or minus change in the eye’s visual environment.
- A plus or minus lens has no effect on the eye’s long-term focus. Nearsightedness cannot be produced in a normal eye by the prolonged wearing of a minus lens.
- The change in focal status of students towards myopia is not related to their increasingly confined visual environment. The development of myopia is due to the genetic make-up of the individual.
A number of these stated predictions have been tested. We feel that the current experimental evidence more strongly supports the concept that the eye is servo controlled versus the concept that the eye is not servo controlled. Actual myopia prevention is a very difficult task to accomplish. This demonstrates that effective myopia prevention is a reasonable expectation, provided the convex lens is assiduously used for all close work. The belief that this approach will work is reflected in current eye care practices [1-4, 19-24, 30-35]. About twenty percent of the profession will use the plus lens (bifocal) to deal with the problem of incipient myopia.
Appendix I: Student Refraction Data R (t) [D], 9 Month Interval.
| Subj | 0 months | After 9 months | ||
|---|---|---|---|---|
| # No. | Begin | Control group | Test group (+) Add | |
| #1 L | -0.75 D | -1.25 D | ||
| R | -0.75 | -1.25 | ||
| #2 L | -0.5 | -1.00 | ||
| R | -1.00 | -1.00 | ||
| #3 L | -0.75 | -1.25 | ||
| R | -1.00 | -1.00 | ||
| #4 L | -0.75 | -0.75 | ||
| R | -0.50 D | -1.00 D | ||
| #5 L | -0.50 D | +0.25 D | ||
| R | -1.25 | +0.50 | ||
| #6 L | -0.50 | +0.50 | ||
| R | -0.50 | +0.25 | ||
| #7 L | -1.00 | +0.25 | ||
| R | -0.50 | +0.50 | ||
| #8 L | -0.50 | +0.25 | ||
| R | -0.75 D | 0.00 D | ||
| < aver> | -0.71875 D | -1.0625 D | +0.3125 D | p< 0.0001 |
| < +/- s.d. > | 0.23935 D | 0.176777 D | 0.17677 D | t = -15.5563 |
| N = 16 | N = 8 | N = 8 | df = 14 | |
Table 2: Student Pilot Refraction Data R(t) [D], 9 month interval
| Subj | Start | After 9 months | ||
|---|---|---|---|---|
| (+) Add Test Group | (-) Control Group | |||
| #1 L | -0.5 D | +0.25 D | ||
| R | -0.5 | 0.00 | ||
| #2 L | -0.5 | +0.25 | ||
| R | -0.75 | 0.00 | ||
| #3 L | -0.5 | +0.5 | ||
| R | -1.00 | +0.25 | ||
| #4 L | -1.00 | 0.00 | ||
| R | -0.75 D | +0.25 D | ||
| #5 L | -0.75 D | -1.25 D | ||
| R | -0.5 | -1.00 | ||
| #6 L | -0.75 | -1.25 | ||
| R | -1.00 | -0.75 | ||
| #7 L | -0.75 | -1.25 | ||
| R | -0.75 | -0.75 | ||
| #8 L | -0.50 | -1.00 | ||
| R | -0.50 D | -1.00 D | ||
| < aver.> | -0.6875 D +0.1875 D | -1.03125 D | t = 12.606 | |
| < +/- s.d.> | 0.19365 D | 0.17677 D | 0.20863 D | p < 0.0001 |
| N=16 | N=8 | N=8 | df = 14 | |
Appendix II: Refraction Data R (t) [D] for Age-Brackets 6 – 18 yrs.
| Age Bracket (+) | Test Group | (-) Control Group | Significance |
|---|---|---|---|
| 6 - 8 yr | +0.06 D, N=22 | 0.65 D, N=102 | p < 0.0001 |
| df=122 | +/- 0.27 D | +/- 0.44 D | t = 7.2654 |
| difference dR = 0.71 D [ 95% CI: 0.52 to 0.90 D ( N = 124 ) ] | |||
| 9 – 10 yr | 0.00 D, N=28 | -0.56 D, N=82 | p < 0.0001 |
| df=108 | +/- 0.23 D | +/- 0.36 D | t = 7.6992 |
| difference dR = 0.56 D [ 95% CI: 0.42 to 0.70 D ( N = 110 ) ] | |||
| 10 – 11 yr | -0.04 D, N=50 | -0.58 D, N = 100 | p < 0.0001 |
| df = 148 | +/-0.16 D | +/-0.37 D | t = 9.8565 |
| difference dR = 0.54 D [ 95% CI: 0.43 to 0.65 D ( N = 150) ] | |||
| 11 – 12 yr | +/- 0.2 D | +/- 0.34 D | t = 7.2773 |
| difference dR = 0.37 D [ 95% CI: 0.27 to 0.47 D ( N = 164 ) ] | |||
| 12 – 13 yr | -0.06 D, N = 56 | -0.59 D, N = 126 | p < 0.0001 |
| df = 180 | +/- 0.17 D | +/- 0.42 D | t = 9.1062 |
| difference dR = 0.53 D, [ 95% CI: 0.42 to 0.64 D (N=182) ] | |||
| 13 – 14 yr | -0.06 D, N = 88 | -0.49 D, N = 74 | p < 0.0001 |
| df = 160 | +/- 0.15 D | +/- 0.3 D | t = 11.8091 |
| difference dR = 0.43 D, [ 95% CI: 0.36 to 0.50 D (N=162) ] | |||
| 14 – 15 yr | -0.03 D, N = 34 | -0.42 D, N = 64 | p < 0.0001 |
| df = 96 | +/- 0.14 D | +/- 0.32 D | t = 6.7585 |
| difference dR = 0.39 D [ 95% CI: 0.27 to 0.50 D ( N=98 ) ] | |||
| 15 – 16 yr | +0.02 D, N = 66 | -0.42 D, N = 50 | p < 0.0001 |
| df = 114 | +/- 0.18 D | +/- 0.33 D | t = 9.1851 |
| difference dR = 0.44 D [ 95% CI: 0.35 o 0.54 D ( N=116 ) ] | |||
| 16 – 17 yr | +0.03 D, N = 36 | -0.39 D, N = 24 | p < 0.0001 |
| df = 58 | +/- 0.2 D | +/- 0.19 D | t = 8.1276 |
| difference dR = 0.42 D [ 95% CI: 0.32 to 0.52 D ( N=60 ) ] | |||
| 17 – 18 yr | +0.21 D, N = 20 | -0.26 D, N = 32 | p < 0.0001 |
| df = 50 | +/- 0.37 D | +/- 0.20 D | t = 5.9490 |
| difference dR = 0.47 D [ 95% CI: 0.31 to 0.63 D ( N = 52 ) ] | |||
| (-) Control Group | (+) Lens Test Group | ||
| Myopia Rates | R’= -0.48 D/yr | R’ = +0.01 D/yr | p < 0.0001 |
| +/- 0.12 D/yr (N=383) | +/- 0.08 D/yr (N=226) | ||
ACKNOWLEDGEMENTS
Partial support for this work was provided by NIH NEI Grant EY 005013 at the Depts. of Biomedical Engineering and Ophthalmology at Johns Hopkins University. The authors would like to thank Jacob Raphaelson, David Guyton, Antonio Medina, Karel Montor and Sterling Colgate for many helpful discussions. Special thanks to Prof. Francis A. Young for providing the Appendix data above.
REFERENCES
- Cheng D, Woo GC, Drobe B and Schmid KL. (2014). Effect of bifocal and prismatic bifocal spectacles on myopia progression in children: three-year results of a randomized clinical trial. JAMA Ophthalmol. 132(3), 258-264.
- Cheng D, Woo GC and Schmid KL. Bifocal lens control of myopic progression in children. Clin Exp Optom. 94(1), 24-32.
- Gwiazda J, Hyman L, Hussein M, Everett D, et al. (2003). A randomized clinical trial of progressive addition lenses versus single vision lenses on the progression of myopia in children. Invest Ophthalmol Vis Sci. 44(4), 1492-1500.
- Scheiman M, Zhang Q, Gwiazda J, Hyman L, et al. (2014). COMET Study Group. Visual activity and its association with myopia stabilisation. Ophthalmic Physiol Opt. 34(3), 353-361.
- Brown O and Berger R. (1979). A Nearsightedness Computer, Proceedings of the Annual New England Bioengineering Conference pp. 343-346.
- Brown OS and Young FA. (1981). The response of a servo controlled eye to a confined visual environment. Biomed Sci Instrum. 17, 41-44.
- Schaeffel F and Howland HC. (1988). Mathematical model of emmetropization in the chicken. J Opt Soc Am A. 5(12), 2080-2086.
- Medina A and Fariza E. (1993). Emmetropization as a firstorder feedback system. Vision Res. 33(1), 21-26.
- Greene PR, Brown OS, Medina AP and Graupner HB. (1996). Emmetropia approach dynamics with diurnal dual-phase cycling. Vision Res. 36(15), 2249-2251.
- Thorn F, Gwiazda J and Held R. (2005). Myopia progression is specified by a double exponential growth function. Optom Vis Sci. 82(4), 286-297.
- Hung GK and Ciuffreda KJ. (2007). Incremental retinal-defocus theory of myopia development--schematic analysis and computer simulation. Comput Biol Med. 37(7), 930-946.
- Medina A. (2015). The progression of corrected myopia. Graefes Arch Clin Exp Ophthalmol. 253(8), 1273-1277.
- Medina A and Greene PR. (2015). Progressive Myopia and Lid Suture Myopia are Explained by the Same Feedback Process: a Mathematical Model of Myopia. J Nat Sci. 1(6), e121.
- Medina A. (2016). Detecting the effect of under-correcting myopia. Graefes Arch Clin Exp Ophthalmol. 254(2), 409-410.
- Greene PR, Grill ZW and Medina A. (2016). Mathematical Models of College Myopia. Optik (Stuttg). 127(2), 896-899.
- Greene PR and Medina A. (2016). Analogue Computer Model of Progressive Myopia–Refraction Stability Response to Reading Glasses. J Comput Sci Syst Biol. 9, 104.
- Greene PR and Medina A. (2016). The Progression of Nearwork Myopia. Optom Open Access. 1, 120.
- Greene PR, Grill ZW and Medina A. (2015). Exploring Reading Glasses to Stabilize College Myopia. J. Sci. Med. Ophthalmology. 3(3), 1034-1039.
- Viikari K. (2011). Learn to understand & prevent myopia. BoD-Books on Demand.
- Goldschmidt E. (2003). The mystery of myopia. Acta Ophthalmol Scand. 81(5), 431-436.
- Nan L, Seger K, Crandall M and Jiang BC. (2010). Effect of customized near addition lenses on transient myopia induced by near-work. Clinical Optometry. 2, 43-49.
- Gmelin RT. (1976). Myopia at West Point: past and present. Mil Med. 141(8), 542-543.
- Brown OS, Young FA and Shotwell AJ. (1982). A predictive mathematical model for the eye’s focal status. Biomed Sci Instrum. 18, 111-116.
- Greene PR, Vigneau ES and Greene J. (2015). Exponential prevalence and incidence equations for myopia. Clin Exp Optom. 98(3), 210-213.
- Young FA, Leary GA, Baldwin WR, West DC, et al. (1969). The transmission of refractive errors within eskimo families. Am J Optom Arch Am Acad Optom. 46(9), 676-685.
- Hooker RJ, Brown OS, Greene PR, Moore JS, et al. (1996). Analog computer simulation of accommodation. In Engineering in Medicine and Biology Society. Bridging Disciplines for Biomedicine. Proceedings of the 18th Annual International Conference of the IEEE. 5, 1777-1779.
- Brown O and Young F. (1980). Physiological Modeling: The Long-Term Growth Of The Eye. Proceedings of the 8th New England Bioengineering Conference. 133-136.
- Brown OS. (2004). How to Avoid Nearsightedness.
- Greene PR, Sergienko NM and Wang SK. (2016). Review: Measurement Techniques for Intraocular Pressure. Optom Open Access. 1(118), 2.
- Young FA. (1961). The effect of restricted visual space on the primate eye. Am J Ophthalmol. 52, 799-806.
- Brown O, Young F and Berger R. (1981). Measuring The Eye’s Focal Accuracy-A Heuristic Approach. IEEE Transactions On Biomedical Engineering. 28(8), 581-581.
- Oakley KH and Young FA. (1975). Bifocal control of myopia. Am J Optom Physiol Opt. 52(11), 758-764.
- Greene PR and Medina A. (2016). Refraction data survey: 2nd generation correlation of myopia. Int Ophthalmol. 36(5), 609-614.
- Fledelius HC. (2000). Myopia profile in Copenhagen medical students 1996-98. Refractive stability over a century is suggested. Acta Ophthalmol Scand. 78(5), 501-505.
- Lin Z, Vasudevan B, Mao GY, Ciuffreda KJ, et al. (2016). The influence of near work on myopic refractive change in urban students in Beijing: a three-year follow-up report. Graefes Arch Clin Exp Ophthalmol. 254(11), 2247-2255.