Previous Issues Volume 1, Issue 2 - 2016
Strategies for Caries Prevention
Michel Goldberg1,2
1INSERM UMR-S 1124, Cellules souches, Signalisation et Prions, 75006 Paris, France.
2Universite Paris Descartes, Sorbonne Paris Cite, UMR-S 1124, 75006 Paris, France.
Corresponding Author: Michel Goldberg, Professor Emeritus, Faculte des Sciences Fondamentales et Biomedicales des Saints Peres, Universite Paris Descartes & INSERM UMR-S 1124. 45 rue des Saints Peres Paris 75006 France, Tel: +33-1-42863851;
E-Mail: [email protected]
Received Date: 17 Sep 2016 Accepted Date: 30 Sep 2016 Published Date: 03 Oct 2016 Copyright © 2016 Goldberg M
Citation: Goldberg M. (2016). Strategies for caries prevention. Mathews J Dentistry. 1(2): 009.
SOME DEFINITIONS: PREVENTION OF THE CARIOUS LESION VS. CLINICAL THERAPY
Prevention of the carious diseases constitutes the preliminary step of caries therapies. It takes place prior any clinical intervention on dental tissues. Preventive options are divided into primary (pit and fissure sealants, and topically applied fluorides including toothpastes and varnishes), secondary and tertiary prevention, involving the patient and professionally [1]. Prevention implies a clear understanding of the characteristics of enamel disorders. It includes the identification of acid-producing bacteria, diet-counseling comprising a long list of fermentable carbohydrates, and host factors, involving teeth and saliva as well.
During the last 30 years, 70 per cent of children aged 5 to 11 years were caries-free, whereas 70 per cent of the 12-17 year-old still had caries [2]. Prevention suggests also an effective role for enamel remineralization. In this context, fluorides play role as key factors for caries treatments. Initial carious lesions of dental enamel may be identified even they may be undetectable. Dental caries processes consists in a bacterial film that produces acids as a byproduct of its metabolism. The acids diffuse through the whole thickness of the dental plaque. Modern methods allow identifying the initial carious decay.
For years, following Black's classification, mechanical rules were applied to teeth preparations. Small area of subsurface demineralization occurs beneath the dental plaque. Drilling creates large cavities prepared according to geometrical requirements. This is required imperatively for the stabilization of the cavity, prophylactic extension, and preparation of horizontal or vertical walls. Mutans streptococci, S. sobrinus and lactobacilli produce lactic acid and appear in plaque before any caries could be clinically observed. Recent spectacular evolutions of dental materials, namely the adhesive properties of resins and glass ionomers, have modified the general concept. As a consequence, this is leading to Minimal Intervention Dentistry. However, different available concepts are determining the rules of Minimal Adhesive Restorations or what is sustaining the preventive concepts implicated in carious diseases.
ENAMEL AND DENTIN CARIES: FROM MINIMAL INTERVENTION DENTISTRY TO PREVENTION IN EVERYDAY CLINICAL PRACTICE
Bacteria are responsible for acid production of dental caries. Dietary fermentable carbohydrates contribute to the dissolution of enamel hydroxyapatite. Due to fluoride intake or to crystal remineralization, the prevention or development of dental caries constitutes a major step for dental caries prevention.
Since the pioneer work of GV Black on operative dentistry, carious lesions are anatomically classified in five classes [3]. The shape and preparation of cavities are related to the anatomical localization of the lesion. Class I concerns exclusively occlusal fissures. Class II develops in the proximal aspects of molars and involves also the occlusal surfaces. Class III affects the proximal surfaces of incisors and canine. Class IV is a mixture of the two previous classes in single-rooted teeth. Cervical lesions, identified as Class V are developing in the collar of teeth, at the junction between enamel, cementum and dentin.
Some rules were adopted during the preparation of cavities, suppressing enamel overhangs, and restraining an easy access to cavities. The limits of the cavities extend up to zones where the cleaning and hygiene of the tooth surfaces may be controlled. They follow architectural rules where only solid dental walls are kept. For decades, these mechanical/biological considerations were mostly related to filling using gold foil, casted inlays, and silver amalgam restorations. Now, adhesive composite resins and glass ionomers have modified the overall concepts, and Black's rules are no more considered as mandatory. Preventing Early Colonization by bacteria seems to be the rule. It comes out that from these historical considerations, two questions arise.
Can we establish a firm diagnosis of the carious decay, which allows determining if prevention will be the predominant nontreatment (non-operative/preventive).
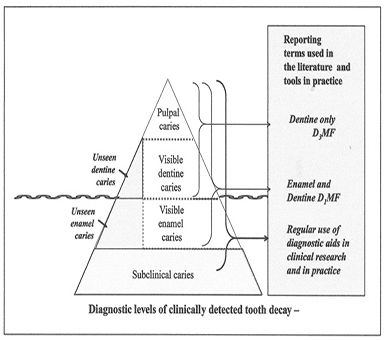
On the other hand, the lesion may need to be cured, following conventional methods routinely used in operative dentistry (Figure 1). The two options may be alternatively used, depending the depth and evolution of the carious lesion.
Figure 1: NB Pitts (Caries Research 2004; 38:294-304) [4].
Visible caries are adapted to Black's concepts developed in most textbooks, allowing restoring the different classes of cavities mentioned above. This leads nowadays to minimal intervention dentistry, which differs from unseen or undetectable carious lesions. These early steps may benefit from prevention.
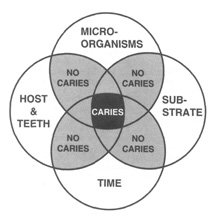
The second question that arises is the following: "Can prevention eliminate caries? [5]. It appears that four main factors are involved in the carious process: the tooth structure (structure, ultrastructure, enamel and cementum defects, the composition of plaque flora, namely the fermentable carbohydrates, and the effects of time). Consequently, four main preventive strategies have been developed: fluorides, fissure sealing, dietary selection and plaque control that differ substantially from minimal intervention dentistry (Figure 2).
Figure 2: Etiological factors in dental caries- in Newbrun 1989 Cariology 3d edition, Chicago [6].
Combining cariogenic factors may contribute to the development of the decay. The suppression of one single factor eradicates or firmly reduces the development of carious lesions.
Using a series of new tools allow to identify the initial carious lesions. Once they are recognized, undetectable or visible early enamel lesions may benefit from technique unmasking early carious lesions and leads to Minimal Intervention Dentistry. Prevention implies another field of knowledge, with huge information on etiologic data, identification of plaque and acid- producing bacteria, diet counseling including fermentable carbohydrates, host factors including teeth and saliva, and opportunities to develop the lesion as a function of time. Prevention uses widely all the chemical agents involved in these specific methods. The combination of information establishes a strong link between the two approaches.
Caries risk factors include dietary habits, poor oral hygiene and dry mouth. Diabetes and Sjogren's syndrome stimulate the development of dental caries. Dry mouth (especially when patients take antimuscarinics drugs), medications that lower the oral pH, and agents inducing demineralization (tetracyclines) are important factors that interfere with the carious development. Consequently, these patients should be advised to visit a dentist regularly.
PREPARATION OF CAVITIES
Instead of drilling with the risk of pulp exposure, preparations may result from spoon-shaped excavators or curettes. According to the dentin caries may be divided into two layers. The outer superficial carious lesion (the soft carious dentin) is "infected" and demineralized, whereas the deeper part of the dentin is "affected" and displays increasing mineralization [8-10]. After the manual elimination of demineralized soft carious dentin, the practitioner reaches the sclerotic dentin surface. Tubules are occluded and partially or totally filled by intraluminal mineralization that either appear as amorphous calcium phosphate or result from crystal formation including whitlookite crystals. These sclerotic surfaces bear also adhesive properties. Between the packed collagen fibrils, the non-collagenous proteins that are present in intercollagenic spaces, may be dissolved by acidic preparation of the surfaces, and/or by adhesives contributing to composite or glass ionomers restorations of caries-free surfaces. Therefore, any geometrical drilled preparation is no more necessary, and even constitutes a danger for the pulp. Adhesive properties became primordial for modern restorative procedures. The shear bond strength is about 10.6 +/- 2.8 MPA, whereas glass ionomer adhesive system provide a significantly lower bond strength (6.5 +/- 1.9 MPA) [11, 12].
The Caries Management System is a non-invasive strategy aiming to arrest and remineralize early carious lesions. It differs intrinsically from preventive strategies.
Table 1: summarizes the ten steps of the Caries Management System [13].
|
1. Diet assessment 2. Plaque assessment (criteria for the Plaque Index according to Silness & Loe, 1964) 3. Bitewing radiographic survey (radiolucency within the outer half, the inner half, beyond the DEJ, in the outer third of dentin, in the inner two third of dentin and if the lesion reach the pulp) 4. Diagnosis and caries risk assessment 5. Preparation of treatment plan 6. Case presentation at which patient is informed about: Dental caries: Arrest Reversal/natural repair (remineralisation), Prevention Number and status of current lesions Role of dental practitioner in caries management Role of home care in caries prevention Current caries risk status Result of diet assessment and recommendations 7. Oral hygiene coaching 8. Topical fluoride application (both professional and home care) 9. Monitoring of plaque control and treatment outcomes at each visit 10. Recall program tailored to caries risk status |
Rules for Filling: Adhesive Properties
The shear bond strength for a glass ionomere such as Vitrabond, or a light cured glass ionomer compared with a glass ionomer liner is 12 +/- 3 MPA versus 4 +/- 2 MPA [14]. These are the reasons why the concepts developed by Black are no more available, and minimal intervention is preferable to drilled cavities, with the risk of pulp horns exposure.
Prevention of Caries
Summarizing, the prevention of dental caries includes:
1. Water fluoridation, leading to -14% caries reduction.
2. Topical fluorides, with obvious differences between the different applications: 24% reduction for fluoride toothpastes, 26% for mouth rinses, 28% for gels, and 46% for varnishes.
The overall benefit was 26% in permanent dentition and 33% in primary dentition [15].
3. Fissure sealants: caries reduction ranging from 86% at 12 months to 57% at 48 months.
This does not lead to the total withdrawal of carious decay, but guide to a firm reduction of the number of lesions.
Using fluorides has reduced the incidence of dental caries, especially when it is given during the critical periods of tooth development. Ingestion of dietary fluorides as supplement increase the risk of enamel fluorosis, namely from birth to age of 36 months. It should be prescribed only for children at high risk of developing dental caries.
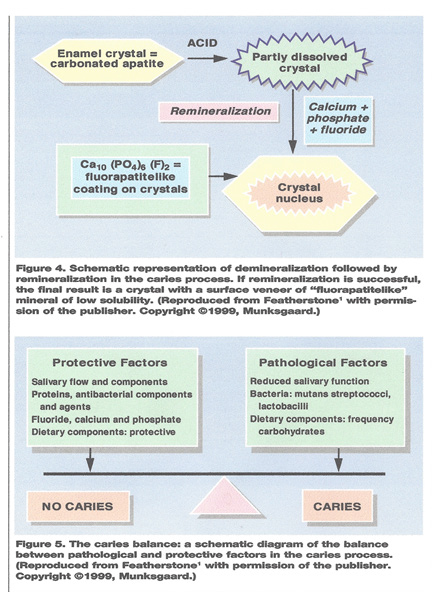
Hydroxyapatite crystals exposed to acids (plaque bacteria) are partially dissolved mostly at their periphery. It has been shown that this is immediately followed by remineralization or reprecipitation of fluoride-rich calcium phosphate, which enhance the resistance to another acidic attack.
Minimal Intervention Dentistry integrates prevention, remineralization and minimal intervention for the placement and replacement of restorations. It implies the least invasive surgical approach, with minimal removal of healthy tissue [16].
Remineralizing agents such as casein phosphopeptide- amorphous calcium phosphate, combined or not to fluoride, novamin, titanium (TiF4 technology), resin infiltrate technology, tricalcium phosphate, nano hydroxyapatite and enamelon have been utilized.
Minimal Intervention
Chemo mechanical preparation of cavity contributes to the elimination of softened carious dentin, removing carious tissue, and pit and fissure associated with the removal of the lesion.
Chemo mechanical cavity preparation implies a number of methods. Caridex is a two-bottle system. The first bottle contains sodium hypochlorite and the second glycine, aminobutiric acid, sodium chloride and sodium hydroxide. Papacarie, involves papain, plasma antiprotease, antitrypsin denaturing collagen molecules, chloramine (acting as thickener) and toluidine blue. Air abrasion may clean the tooth surface with aluminium oxide particles carried in a stream of air. Ultrasonic Instrumentation and soon-abrasion offer facilities to remove carious decay. Ozone and lasers may be used for hard tissue management.
Toothpastes (dentifrices), Mouthwashes, Memineralization/ Caries Arrestment
Dentifrices are effective anti-caries agents. They include dentifrice abrasive such as calcium carbonate, dicalcium phosphate, silica, and /or sodium bicarbonate. Some agents inhibit calculus formation. Pyrophosphate is an inhibitor, but also interfere with the remineralization process. The length of the application phase determines how long the fluoride concentration in the dentifrice slurry stays in contact with the teeth and plaque. High fluoride concentration allows greater driving force for fluoride diffusion through plaque toward the tooth surface.
Amorphous Calcium Phosphate (ACPs) and NaF prevent root caries. They are influencing remineralization. However, the small number of study doesn't allow establishing the efficacy of methods. Most remineralization is limited to the surface of carious lesions.
Some caries arrested agents may be topical. They include silver nitrate, stannous fluoride, sodium fluoride, silver fluoride and silver diamine fluoride. They prevent further caries progression, referred as Atraumatic Restorative Treatment (ART). Without local anesthesia, the carious tissue is removed with hand instruments and the lesion is restored with Glass Ionomer Cement. Mouthwashes with chlorhexidine may also contribute to carious reduction. Other bacteria inhibitors may contribute efficiently to caries reduction.
Fluoride compound, concentration, frequency of use, duration of exposure, and method of delivery can influence fluoride efficacy. Fluoride dentifrices are the most widely method of delivering topical fluoride. Fluorides may arrest carious lesions with or without prior removal of carious tissue. This is included in the Traumatic Restorative Treatment (ART).
| Recall protocol | schedule for monitoring caries activity |
| Caries risk | Caries activity |
| Low |
|
| Medium |
|
| High |
|
| lesion progression has arrested/reversed and patient is reclassified as medium/low risk. | |
Fluoride Remineralization Intend to Arrest Dental Caries
The use of 5000ppm in the drinking water is 30-40 % more effective than 1000 ppm. Reduction per 1000 ppm produces 12.7% caries reduction (DMFS) when added in toothpaste. 2500-2800ppm is 15-20% more effective than 1000 [17, 18]. There is strong evidence based on the use of high fluoride toothpastes in groups of greater risk of caries. It has reported that children aged 9 years living in North Dakota with 1.7 to 2.5 ppm F in the drinking water had only 2.0 decayed teeth, while those in countries with 0.6 to 1.5 ppm F had 4.2 decayed teeth [19].
Fluoride is still the most-effective caries-preventing anticaries and remineralizing agents. Toothpastes, chewing-gums, and rinses are very effective for fluoride delivery.
Anti-microbial therapies acting on the biofilm may contribute to prevention. Fluoride at 0.04ppm in saliva can enhance remineralization. Milk fluoridation is useful in the range of 0.5 to 1.0 mg/day. In such conditions, a precise amount of fluoride can be delivered under controlled conditions [20]. Incubation of root dentin with fluoridated milk showed a clear effect on root dentin remineralization. Incubation with NaF dissolved in artificial saliva demonstrated a stronger effect [21].
At least 10 reports confirmed the caries-protective effect of 1.0ppm F in the drinking water [22].
Pit and fissure sealants are used for the prevention and management of caries. They should be considered to prevent dental caries. Molars have many groves (fissures) and pits that are susceptible to develop decay. Priority should be given to sealing first and second permanent molar teeth. They should be used for selected high-risk children. Sealants should be applied as soon as the tooth is sufficiently erupted to be isolated by a rubber dam. Sealants should be placed on permanent teeth without cavitation as soon after eruption as isolation can be achieved. Sealants should not be placed on partially erupted teeth or teeth with cavitation of caries of the dentin. Sealant should be placed on permanent teeth within 4 years after eruption.
Pit and fissure sealants (ultraviolet-activated, auto polymerized or light cured resin-based (RB) sealants, or glass ionomer (GIC) cements have been developed in the 1970s and 1980s, and it is obvious that these materials are effective in preventing caries. RB materials are more effective than GIC materials [23]. It is important to adequately isolate the teeth. Salivary contamination is the major cause of loss of sealants in the first year.
Resistance to Bacteria. Caries-Associated Microorganisms Streptococcus mutans and S. sobrinus are the major cariogenic bacteria. Lactobacilli species are producing lactic acid and appear in plaque before caries may be clinically observed. Fluoride inhibits bacterial metabolism, inhibits demineralization and enhance remineralization. Fluoride inhibits enolase, an enzyme necessary for the bacteria to metabolize carbohydrate.
Antibacterial properties of composite and adhesive systems lead to biofunctional materials. Some dentin bounding, which contain glutaraldehyde or have acidic properties, exhibits some antibacterial effects. These modifications have advantages and contribute to the production of useful materials [24].
Saliva
Salivary flow rate, buffering capacity and pH.
Hyposalivation is one of the strongest indicators for an increased risk of dental caries. After irradiation or in the elderly, salivation is reduced. Psycho-pharmaceutical products reduce the flow rate and affect the caries risk. Pharmacological or electrical stimulation, salivary substitutes, mineral water (St Cristau water), or drugs may influence the saliva reduction, and therefore counterbalance the effects of liquid reduction on the development of rampant caries, on plaque accumulation and eventual dissociation.
Bacteria
Bacterial tests are based on the premise that saliva levels represent levels in oral biofilm. Streptococci mutans and lactobacilli predict the salivary flow rate. Bacteria present in cervical and interproximal areas are associated with gingivitis. But also there are risks areas for patients and caries development.
Mutans streptococci have long been assumed to be specific pathogen of the dentin caries. The relative abundance of Lactobacillus (high, middle, low) [cluster I], and Prevotella are associated with Propionibacterium [cluster II]. Some samples in cluster III reveal novel combinations of microbiota in carious dentin lesions.<> The risk is increased with the presence of stagnant mature plaque. The importance of mutans streptococci (including S. mutans and S. sobrinus) in the development of dental caries has been extensively established. It is well documented that a greater number of mutans streptococci and lactobacilli in saliva are associated with high caries rates.
Immunization against caries has been one of the targets. IgA produced by the saliva can interfere with the colonization of the surface of the tooth by specific bacteria.
Sugar Substitutes
In case of rampant caries, profoundly caries-susceptible tooth structure, poor diet, hyposalivation, amelogenesis imperfecta, etc., the use of non-cariogenic sugar substitutes should automatically be considered. Fermentable carbohydrate has been implicated in the development of caries, even in case of low sugar intake.
Sorbitol- and xytlitol-sweetened chewing gum may control the development of caries. These sugar substitutes play role in caries prevention. Sorbitol-sweetened gum, had low cariogenicity when chewed no more than three times per day.
Xylitol is a sweet crystalline carbohydrate, derived from xylose. It is classified as similar to sorbitol and mannitol. Cariogenic micro- organisms do not metabolize xylitol. Xylitol as a potential caries-limiting and an anticariogenic dietary sweetener. Dietary xylitol improves calcium absorption and prevents osteoporosis. No decrease of pH is noticed. There is no plaque accumulation. Chewing xylitol-sweetened gum three to five times per day for a minimum of five minutes after meals inhibits plaque accumulation and enamel demineralization, enhances remineralization of early lesions and reduces mutans streptococci counts [25]. Rampant caries are stabilized, and rehardening processes have been noticed. Hyposalivation or dry-mouth syndrome (Sjogren's syndrome) benefits from the systematic usage of xylitol-containing saliva stimulants. Xylitol is not a panacea, but an effective adjunct to "caries prevention programs" [26].
However, epidemiological studies don't demonstrate accurately that a drastic reduction in sugars intake do not provide unequivocally data on the cariogenicity of sucrose or even very low monosaccharide intake. According to Sheiham and scientific confusion arises from the pressure of major industrial sugar interests [27]. Recently, the proposal from the National Caries Program to restrict sugar consumption in order to prevent caries was excluded [28].
Understanding the balance between pathological factors and protective factors is the key. Methods including fluoride therapies for inhibition of demineralization and enhancement of remineralization seem to be crucial. Altogether the technologies require the way in which dentist diagnose, intervene, treat and manage caries for the benefit of the oral health of patients.
-
REFERENCES
- Longbottom C, Ekstrand K and Zero D. (2009). Traditional preventive treatment options. Monogr Oral Sci. 21, 149-155.
- Featherstone JDB. (2000). The science and practice of caries prevention. JADA. 131(7), 887- 899.
- Black GV. (1908). Operative dentistry. 1.
- Pitts NB. (2004). Are we ready to move from operative to non-operative/preventive treatment of dental caries in clinical practice? Caries Res. 38, 294-304.
- O'Mullane D. (1995). Can prevention eliminate caries? Advances in Dental Research Adv Dent Res. 9(2), 106- 109.
- Newbrun E. (2006). Cariology. Williams & Wilkins Baltimore/ London. 232-245.
- Zero DT. (2006). Dentifrices, mouthwashes, and remineralization/ caries arrestment strategies. BMC Oral Health. 6(Suppl 1), 59.
- Fusayama T, Okuse K and Hosoda H. (1966). Relationship between hardness, discoloration, and microbial invasion in carious dentin. J Dent Res. 45(4), 1033-1046.
- Massler M. (1967). Pulpal reactions to dental caries. Int Dent J. 17(2), 441-460.
- Fusayama T and Terachima S. (1972). Differentiation of two layers of carious dentin by staining. J Dent Res. 51(3), 866.
- Bishara SE, Gordan VV, VonWald BA and Jakobsen JR. (1999). Shear bond strength of composite, glass ionomer, and acidic primer adhesive systems. Am J Orthod Dentofacial Orthop. 115(1), 24-28.
- Meerbeek BV, Munck DJ, Yoshida Y, Vanherle G, et al. (2003). Adhesion to enamel and dentin: current status and future challenges. Operative Dentistry. 28-3, 215-235.
- Evans RW, Pakdaman A, Dennison PJ, Howe ELC, et al. (2008). The caries management system: an evidence-based preventive strategy for dental practitionners. Application for adults. Australian Dental Journal. 53(1), 83-92.
- Mitra SB. (1991). Adhesion to dentin and physical properties of a light-cured glass ionomer liner/base. J Dent Res. 70(1), 72-74.
- Watt RG. (2005). Strategies and approaches in oral disease prevention and health promotion. Bulletin World Health Organization 83(9), 711-718.
- Jingarwar MM, Bajwa NK and Pathak A. (2014). Minimal Intervention Dentistry- a new frontier in clinical dentistry. J Clinical & Diagnostic Research. 8(7), ZE04-ZE08.
- Pretty IA. (2016). High fluoride concentration toothpastes for children and adolescents. Caries Res. 50(suppl 1), 9-14.
- Featherstone JD. (1999). Prevention and reversal of dental caries: role of low level fluoride. Community Dent Oral Epidemiol. 27 (1), 31-40.
- Dean HT. (1938). Endemic fluorosis and its relation to dental caries. Public Health Rep. 53(33), 1443-1452.
- Banoczy J, Rugg-Gunn A and Woodward M. (2013). Milk fluoridation for the prevention of dental caries. Acta Medica Academica. 42 (2), 156-167.
- Arnold WH, Heldt BA, Kuntz S and Naumova EA. (2014). Effects of fluoridated milk on root dentin remineralization. Plos One. 9(8), e104327.
- Marthaler TM. (2013). Salt fluoridation and oral health. Acta Medica Academica. 42(2), 140-155.
- Azarpazhood A and Main PA. (2008). Pit and fissure sealants in the prevention of dental caries in chilfren and adolescents: a systematic review. JCDA. 74(2), 171-177.
- Imazato S. (2003). Antibacterial properties of resin composites' and dentin bonding systems. Dental materials. 19(6), 449-457.
- Burt BA. (2006). The use of sorbitol- and xylitol-sweetened chewing gum in caries control. 137(2), 190-196.
- Peldyak J and Makinen KK. (2002). Xylitol for caries prevention. J Dental Hygiene. 76(4), 276-285.
- Sheiham A and James WPT. (2015). Diet and dental caries: the pivotal role of free sugars reemphasized. J Dent Res. 94 (10), 1341-1347.
- Kearns CE, Glantz SA and Schmidt LA. (2015). Sugar industry influence on the scientific agenda of the National Institute of Dental Research's 1971 National Caries Program: a historical analysis of internal documents. PLoS Med. 12(3), e1001798.